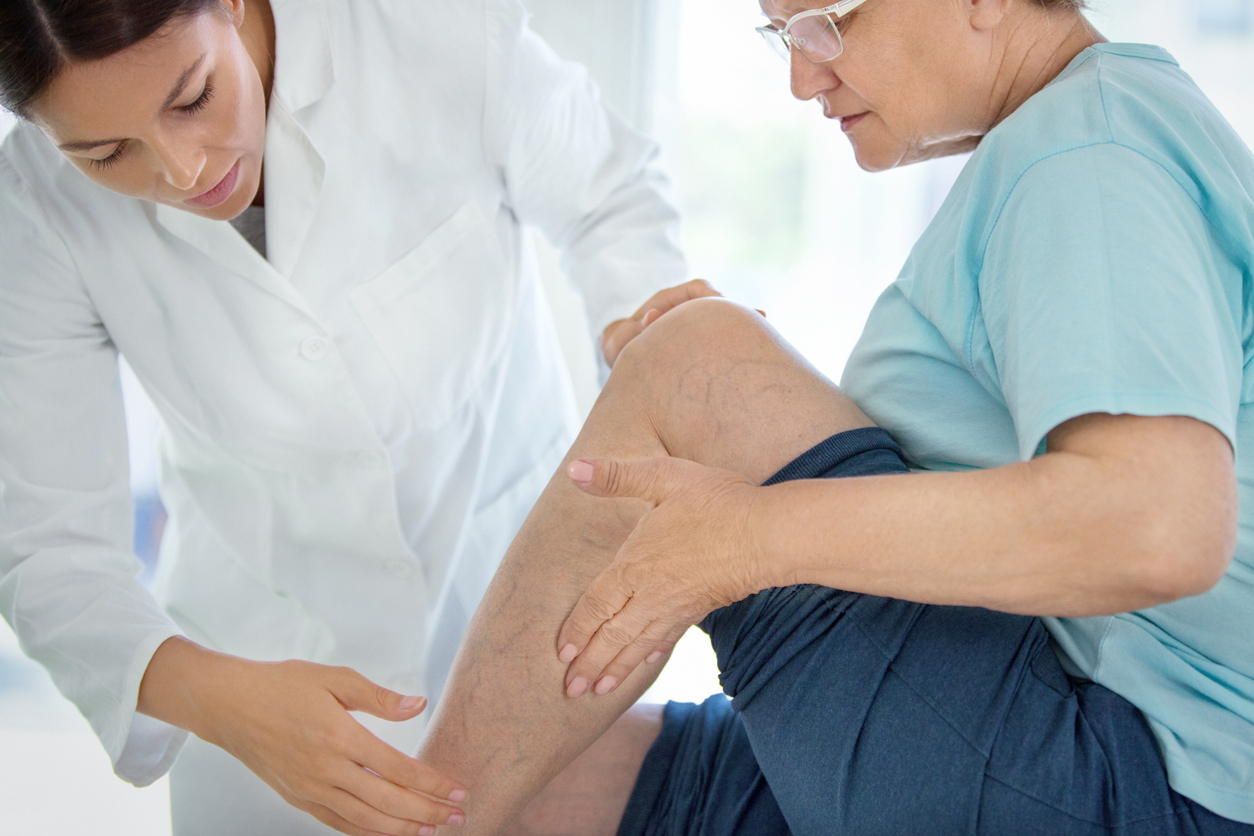
Varicose veins and spider veins are unsightly and uncomfortable conditions that affect many people, and, in the case of varicose veins, they can lead to serious complications. To help alleviate the symptoms of varicose veins, you may consider laser or surgical procedures that are designed to relieve pressure on the veins and promote better circulation.
Fortunately, there are many different types of vein treatments to choose from, and they can all be performed on-site at a vein treatment clinic. The recovery time is minimal as well, so you’re able to return to your normal routine in no time.
If you’re considering vein treatment, take a look at this guide to vein conditions, vein treatments and what to expect before, during and after your surgery.
Continue reading

Also known as Willis-Ekbom Disease, Restless Leg Syndrome (RLS) is a condition that’s characterized by unpleasant and uncomfortable sensations in the legs and an uncontrollable urge to move them. Restless leg syndrome has many possible causes, including venous disease, and effective treatment revolves around managing the symptoms to improve quality of life. So, if you’re suffering from RLS and are diagnosed with an underlying venous disease, there is hope for treatment and relief of symptoms.
While the severity may differ between affected individuals, most patients report symptoms that occur in the late afternoon to evening hours, with the worst effects occurring at night when the patient is resting. This can also occur when the patient is inactive or sitting for long periods of time, such as on a road trip.
Because the condition worsens during the night, RLS can cause sleep disturbances and difficulty returning to sleep after arousal. In many cases, moving the legs or walking can temporarily relieve the discomfort, but the sensations return once the movement stops.
RLS is classified as a sleep disorder, due to the symptoms being triggered by resting and worsening in the evening, and a movement disorder, since patients are forced to move in an effort to relieve discomfort. Though these classifications apply, RLS best fits the category of neurological-sensory disorder, since the symptoms and underlying condition are caused by the brain.
Continue reading
Approximately 1 in 4 adults suffer from varicose veins, the bulging, twisted veins that appear on the thighs, calves and feet. Varicose veins can be uncomfortable and unsightly, not to mention the burning, throbbing, cramping and swelling that many patients also experience.
Fortunately, the Venefit procedure is the latest development in varicose vein treatment, which can get rid of unpleasant veins with minimal discomfort and recovery time.
Find out more about the benefits of the Venefit procedure and how it can end your varicose vein and leg discomfort for good in today’s blog.
Continue reading
Varicose veins are often a painful condition. Your veins may become enlarged as a result of abnormalities in venous circulation. Varicose veins are typically located on the lower legs, and many people with this condition find them unsightly. In addition to the protrusion and discoloration of the veins on your legs, you can also experience heaviness and achiness in the legs, which can make work and daily activities much more difficult than it should be.
Fortunately, treatments are available for varicose veins that have proven to be effective. Two of the most popular treatments are endoscopic venous laser therapy (EVLT) and radiofrequency ablation (RFA). Learn more about your options and get an idea of which might be best for you with this handy EVLT vs. RFA comparison.
Continue reading