7 Signs that You Need to Visit a Vein Specialist to Treat Your Vein Disease
Varicose vein disease and other forms of venous insufficiency are prevalent in many countries around the world. For instance, in the United States an estimated 30 to 40% of the population suffer from varicose veins. Approximately 41% of women will have abnormalities in their leg veins by their 50’s, and 60% of all American men and women will experience some form of vein disorder in their lifetime.
Many of those who suffer from vein disease (in other words, veins that stop functioning as they should, especially with regard to blood circulation) deal with discomfort, aching, and even pain on a daily basis. Still, they may be reluctant to seek treatment from a qualified medical professional. Perhaps they feel that a doctor would not be able to effectively help them. They may worry about the financial cost of treating the disease. In addition, they may fear that treatment options will be painful.
Many sufferers believe that home remedies are sufficient to deal with their vein disorder. These home remedies may include wearing tight stockings; however, tight stockings do not serve as an effective treatment for vein disease. While graduated compression stockings specifically designed to combat venous disease can promote good vein function and health, they cannot cure the disease. Other common home remedies include the application of certain oils and herbs to the affected area, such as olive oil, garlic, or witch hazel.
If you are using home remedies to fight vein disease, then you are not alone. Nevertheless, there are definite signs that indicate you need to move past home remedies and seek the help of a qualified vein specialist. In the following information, we will discuss the 5 main stages of vein disease, 7 key indicators that it’s time to visit a vein disease expert, and some of the treatment options available to patients today.
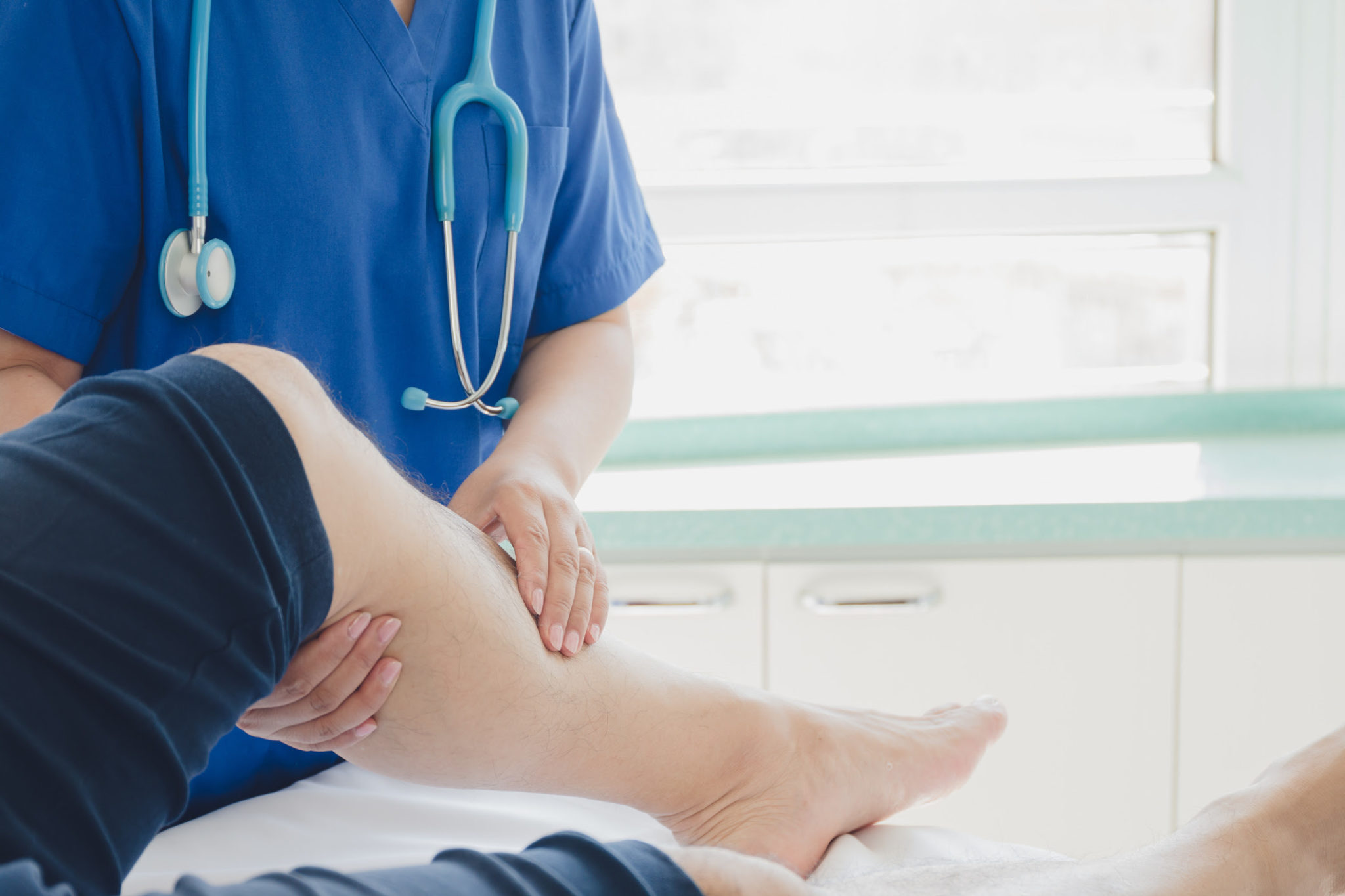
The 5 Visible Stages of Vein Disease
Vein disease is a progressive condition, which means that you should be alert to early signs of any venous disorder or insufficiency. In many patients, the first stage of vein disease manifests in symptoms such as tired, restless, or aching legs; or itching, burning, and swollen ankles. Nevertheless, there may not be visible signs of vein disease at this stage. The patient with these symptoms should consider seeking consultation, even though no abnormal veins may be visible.
With regard to the visible manifestations of vein disease, the progression can be divided into 5 main stages:
- Spider veins (reticular veins). Spider veins are formed when tiny veins congregate beneath the skin’s surface and cause visible discoloration (typically red, blue, or purple). They typically manifest on the legs or face, and are at most 1.5 millimeters in size. (Reticular veins, which are a slightly larger type of spider veins, may get as large as 3 millimeters, and often form in cascades.) There are a number of factors that lead to the formation of spider veins, including heredity, body weight, occupation (if it involves standing for long periods of time) and hormonal changes. While spider veins are generally considered harmless, they (along with varicose veins) present as the beginning stage of more serious venous issues.
- Varicose veins. In contrast to small spider veins, varicose veins are larger and more visible (at least 3 millimeters in size). They usually occur in the legs. Like spider veins, varicose veins are branches of the body’s superficial venous system. They may cause symptoms that include itching, burning, cramping, or throbbing in the legs, especially around in the areas immediately surrounding the varicose veins. Varicose veins tend to further deteriorate without appropriate treatment, leading to more serious health issues.
- Inflammation (usually of legs and/or ankles). The formation of varicose veins often leads to the inflammation (aka swelling) of the legs and/or ankles. This is because the blood that should be circulating back towards your heart is instead accumulating or “pooling” within the varicose veins. Swelling is often accompanied by a range of other symptoms, including itchy legs, tightness in the ankles or calves, pain when walking, muscle spasms, and restless leg syndrome. Sometimes patients can gain relief from symptoms by raising their legs above their hearts. Swollen legs and ankles may mark the onset of chronic venous insufficiency (CVI) disease. Thus, it is important to seek out a proper diagnosis before the condition worsens.
- Lipodermatosclerosis (skin discoloration). In the fourth stage of vein disease, the skin around the varicose veins will begin to turn a different color (usually brown), crack, bleed, and swell. At this point, the affected area is usually itchy and irritable. In addition, previous symptoms of vein disease may present with a higher amount of pain.
- Ulcers and open sores. Ulcers are sores that do not heal, but instead continually reopen. In this stage of venous disease, ulcers will form on the exterior of a patient’s skin due to the buildup of pressure within the veins. These ulcers can be quite painful. In addition, patients may also experience burning legs, leaking veins, and all of the previously mentioned symptoms from earlier stages of the disease.
It is important to note that an accurate diagnosis from a qualified medical professional, along with appropriate treatment, may halt the progress of a patient’s venous condition and in some cases even reverse its effects.
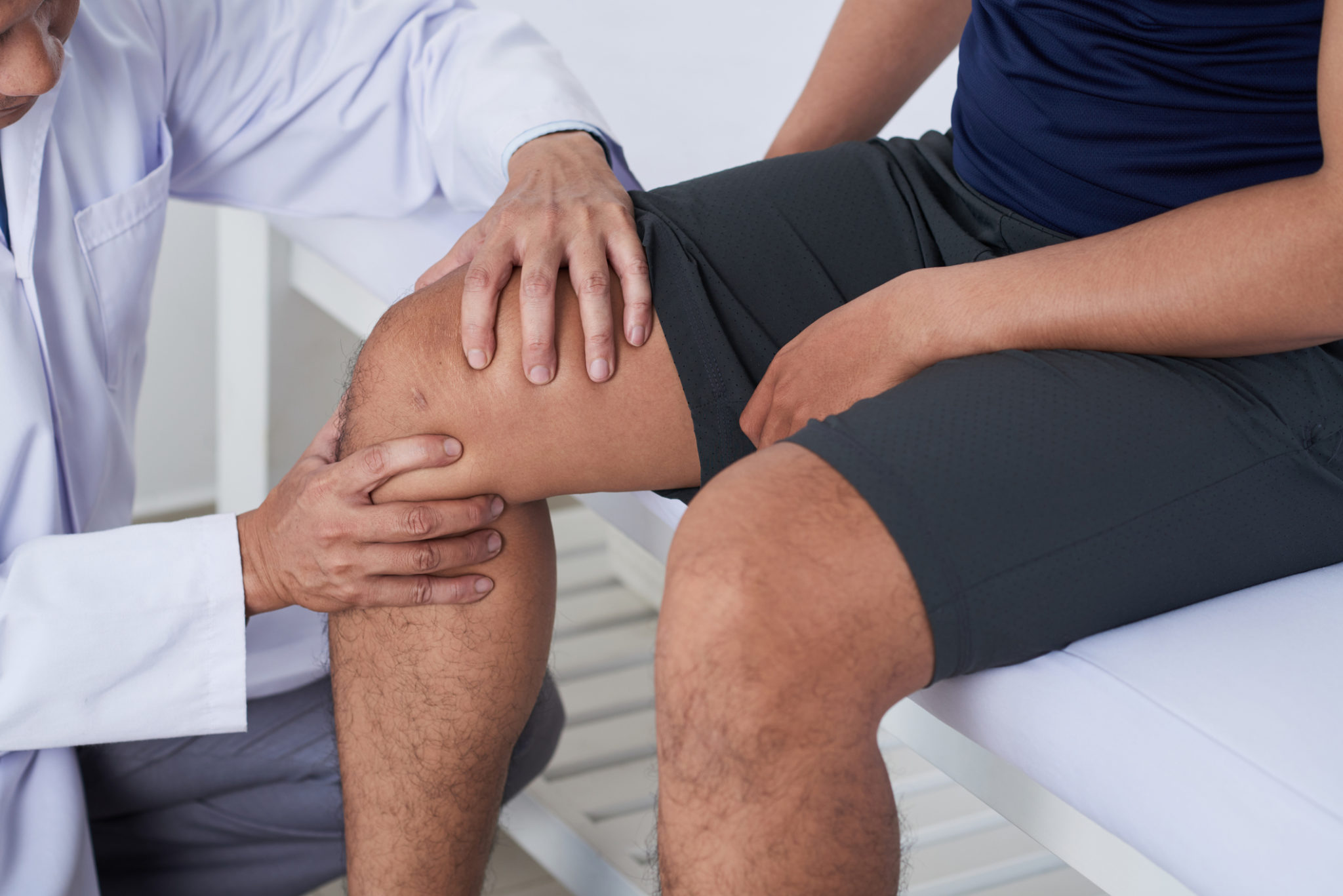
7 Signs that You Should Visit a Vein Specialist
There are several indicators that should alert you when it is time to take action, and visit a vein specialist. 7 key signs are discussed below:
1. Weakness in Your Legs
Many jobs today involve standing for long periods of time, sometimes for almost an entire 8 or 10 hour shift. The problem with such posture is that without adequate movement of the legs, it becomes very difficult for the leg muscles to generate the upward force needed to ensure sufficient circulation back to the heart.
If you are experiencing weakness or tiredness in your legs after standing in the same position for a long time, then this may be one of the early symptoms of vein disease. Acute or occasional leg pain in particular could indicate some form of venous insufficiency.
2. Chronic Leg Pain
It is true that not all leg pain is a result of venous insufficiency. Nevertheless, aching, throbbing, muscle cramps, and chronic pain in the legs are symptoms commonly associated with vein disease.
Many sufferers mistake such symptoms as side effects of tiredness, overexertion, lack of fitness, or advancing age. However, it is usually best to err on the side of caution and visit a vein specialist to get an accurate diagnosis. Mild pain as a result of venous insufficiency can often be addressed with compression stockings. Otherwise, the specialist can recommend a number of treatment options to help you find relief from daily leg pain.
3. Leg Ulcers
As discussed above, leg ulcers usually develop in the later stages of vein disease. These painful, recurring sores are typically common around the medial or inner calves and inner ankles.
While diabetes is another leading cause of leg ulcers, an experienced vein doctor can run tests to uncover the source of the problem in your case.
4. Pregnancy
The blood volume in a pregnant woman generally increases by 30% or more in order to support the growing fetus. However, much of this additional blood volume may begin pooling due to an increase in pressure.
In pregnancy (especially the later stages) the pressure of the growing uterus on the pelvic veins causes blood volume to back up into the legs. The legs often become tremendously swollen. The veins become so enlarged, so stretched, that the flap valve mechanisms are disrupted and may never close properly again – even after delivery of the baby. Thus, pregnant and postpartum mothers may find the services of a professional vein doctor to be helpful.
5. Blue or Purple Veins that Bulge Out
If your veins begin to noticeably bulge outward from your skin, or turn a blue or purple color, then you may need to get a diagnosis from a qualified vein specialist. Such symptoms are caused by the inflammation of your varicose veins. At this point, there is a small possibility that you could develop a blood clot, thus completely halting blood flow through the vein.
It is important to seek out proper treatment for this condition as soon as possible. Superficial venous thrombophlebitis is extremely painful, and often causes the leg to become red and inflamed. An experienced vein doctor can take the necessary steps to treat this painful complication and restore your quality of life.
6. One Swollen Leg
While there may be a number of reasons for your legs to swell, if only one leg is affected by swelling or inflammation, if this only occurs after you’ve been awake and ambulatory for a while, and if the swelling disappears overnight, then it is likely that some kind of venous insufficiency is involved. Again, a visit to an experienced vein doctor can confirm that vein issues are the root cause of your swelling.
7. A Tender Lump in Your Leg
Blood clotting in your veins often results in the development of a tender lump in the surrounding area of your leg. If you notice that such a lump has developed on one of your legs, then it may be a good idea to contact a vein specialist.

Treatment Options for Vein Disease
Treatment plans for vein disease generally fall into one of seven different categories. The majority of these categories involve pain-free and/or minimally invasive techniques to deal with venous issues. These categories include:
- Compression stockings. This conservative treatment option involves wearing tight-fitting support stockings that are designed to assist in the upward circulation of blood back towards the heart. These stockings are available for purchase at most surgical supply stores, and come in 3 basic varieties: below the knee, above the knee, and pantyhose.
- Changes in lifestyle. Many vein issues are directly correlated with certain lifestyle habits. Your doctor may encourage you to make appropriate lifestyle changes. These could include weight loss and regular exercise.
- Sclerotherapy. This outpatient procedure is quick, simple, and fairly inexpensive. It often involves the injection of polidocanol (aka Asclera) into the target vein, although sodium tetradecyl and hypertonic saline are also utilized. The Asclera causes the vein to scar and eventually collapse, thus rerouting blood flow back to healthy veins. The vein itself disappears over a period of three to six weeks. The entire procedure may last less than an hour.
- Endovenous Laser Treatment (also known as EVLT). In this outpatient procedure, a small laser fiber is inserted into the varicose vein. The laser heats the blood in the vein with reflux, leading to changes that ultimately result in the closure of the vein. Only local anesthesia is required for this treatment; however, it can be quite a painful operation.
- Radiofrequency Ablation (RFA). Radiofrequency ablation is another outpatient procedure. It involves the insertion of a small catheter into the targeted vein. The catheter converts radio frequency to heat at its active segment. This segment directly contacts and heats the vein wall, leading to changes in vein wall proteins and the closure of the vein. Eventually the vein is attacked by white blood cells and turned into a flimsy piece of scar tissue that is not visible or palpable to the patient in the long run. When the vein is ablated, the blood returns toward the heart by following a pathway of working veins that contain working valves.
- Traditional vein surgery (aka formal vein ligation and stripping). Traditional vein surgery is painful and debilitating, often causing patients to lose weeks of work. Vein stripping is emphatically not an acceptable solution for any problematic veins that are visible on ultrasound and treatable with one or more of the aforementioned minimally invasive approaches. Simple ligation through multiple small incisions can be initially gratifying, but is typically a failure in the long run because the source of reflux in untreated, unstripped veins simply finds other areas to reflux into, thus causing more varicose veins and painful symptoms.
- Lasers/intense pulsed light. Procedures that involve surface laser or pulsed light devices use heat energy to eliminate abnormal veins. While no needles or sclerotherapy solutions are required for these operations, patients may experience minor discomfort as well as disappointing results.
Reach Out to an Experienced Vein Specialist
If you suspect that you are suffering from some form of venous insufficiency, don’t delay. An experienced, qualified medical professional can help you to cope with your current symptoms, prevent future problems, and live a healthier life.
At Vegas Valley Vein Institute, Dr. Irwin B. Simon, MD and his team of caring vein specialists is here to provide you with the support that you need. If you have any questions related to vein disease, contact us today. We’d be happy to assist.