Varicose Veins: Topical, Surgical, and Minimally Invasive Treatment Options
Healthy veins remove waste products and direct blood flow to your heart and lungs. A series of valves lining the inside of your veins keeps your blood moving against the pull of gravity. As your muscles contract, the valves open to keep blood moving forward. When muscles relax, the valves close to keep blood from flowing in reverse.
Varicose veins are most often the result of valve damage. Once a valve fails to close securely, a condition known as venous insufficiency, leaking valves allow blood to flow downward towards your feet. When damage occurs in the tiny blood vessels near the surface of your skin, you will likely notice the familiar web-like configuration of spider veins (telangiectasia). When larger veins are affected, the veins below the damaged valves can bulge, twist, and cause a significant amount of discomfort.
Unfortunately, far too many people living with the discomfort of varicose veins unnecessarily delay medical intervention. Some put off having their varicose veins treated because they don’t think their veins are damaged enough to justify treatment. Others mistakenly assume they would have to dedicate a significant amount of time to recover after surgery. While surgery is still the best option in some cases, doctors today are more likely to recommend minimally invasive varicose vein treatment.
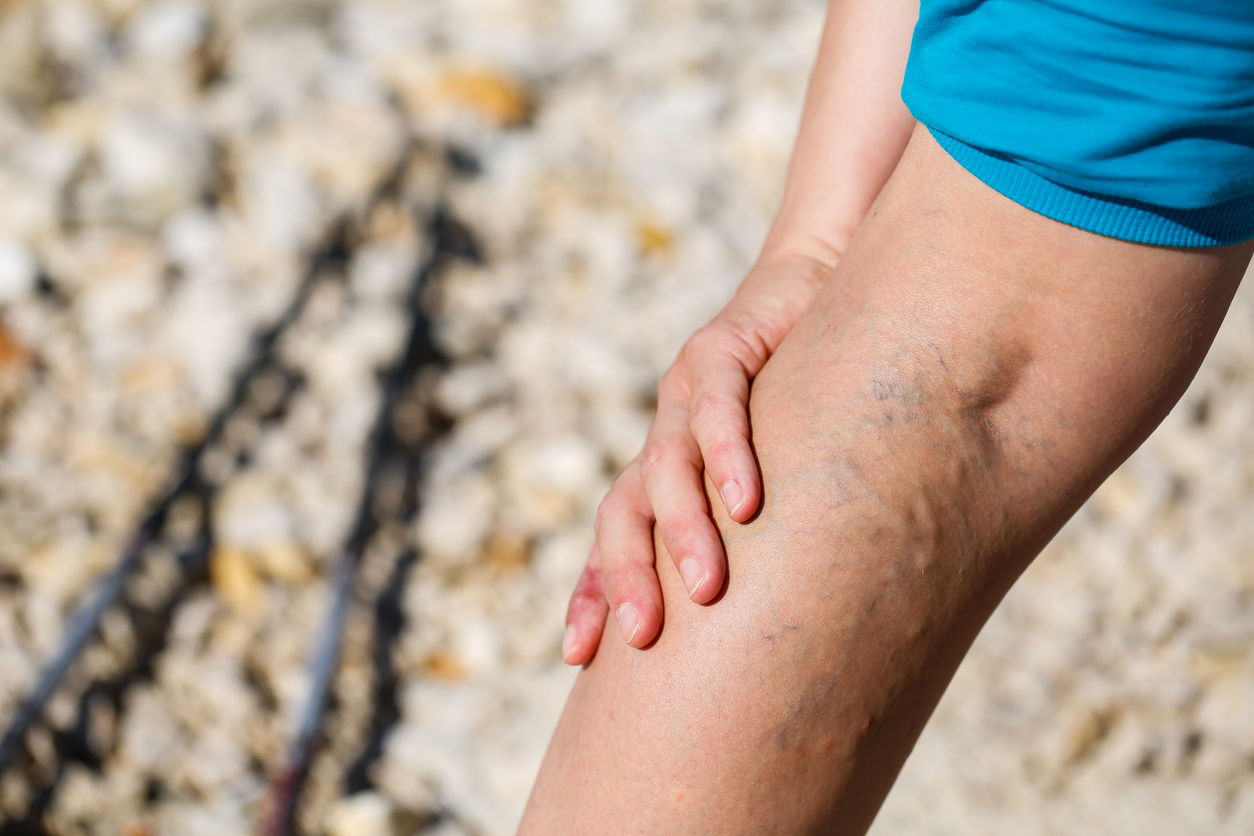
The Factors Contributing to Venous Insufficiency
While varicose veins (and spider veins) can appear anywhere on your body, they most commonly appear on the lower leg or pelvic region. Most will develop near the surface of your skin. While bulging, twisted veins are not considered a serious medical problem on their own, untreated varicose veins can cause a significant number of health complications.
As circulation deteriorates around the affected blood vessels, venous insufficiency can cause swelling in the legs, skin discolorations, and venous stasis ulcers. Just a few of the many factors that could contribute to developing venous insufficiency include:
- A family history of varicose veins
- Medical conditions that increase abdominal pressure (liver disease, heart failure, groin surgery)
- Injury to the veins
- Being overweight
- Hormonal fluctuations during pregnancy
- Hormonal changes caused by birth control or hormone replacement therapy
- Professions that require prolonged sitting
- Professions that require prolonged standing
An estimated one-third of our population over the age of 45 has some form of vein disease. That percentage steadily increases with age. While most people initially consider varicose veins little more than a cosmetic concern, eventually those bulging, dilated, twisted blood vessels interfere with healthy circulation.
Varicose Veins Can Cause a Significant Amount of Discomfort
Not everyone with varicose veins develops debilitating symptoms, but it’s important to realize that once varicose veins develop they will not resolve on their own. As healthy circulation declines, fluids can accumulate in surrounding tissues and lead to a significant amount of discomfort. If you have varicose veins, you are likely aware of one or more of the following symptoms:
-
A Feeling of Heaviness in Your Legs
When you have varicose veins, the accumulation of fluids in your veins can cause your legs to feel heavy or tired. You may notice that walking or standing can make your tired legs feel significantly worse. Elevating your legs periodically for 10-15 minutes throughout the day can take some of the pressure off of your veins, improve your circulation, and could help you feel more energized.
-
Swelling of the Affected Limb
Venous insufficiency and the resulting varicose veins are the most common causes of fluid accumulation (edema) in the legs. As blood pools in damaged areas, your veins are likely to take on more fluid than they can withstand. The increased pressure causes your veins to expand and stretch. With increased pressure on diseased veins, the smaller blood vessels begin to leak proteins, plasma, and waste into surrounding tissues. Your swelling is the result of tissue expansion caused by fluid retention.
-
Nocturnal Leg Cramps
Research shows that people who have varicose veins experience nocturnal leg cramps more frequently than those who do not have varicose veins. The increase in frequency is most likely due to decreased blood flow to the affected muscles, particularly to the muscles of the calf. Researchers discovered that 78 percent of those living with varicose veins experience nocturnal leg cramps compared to 52 percent of those surveyed who did not have varicose veins, regardless of age.
-
Skin Discoloration, itching, and Rashes
As the symptoms of vein disease progress, you may notice considerable changes in the texture and color of your skin, particularly the skin of your lower leg. The discoloration is the result of the breakdown of blood cells that leak from the smaller blood vessels closest to the surface of your skin. As blood cells break down, you could find that your lower leg turns various shades of red or brown. In addition to the changes in the color of your skin, varicose veins can compromise healthy circulation and impair your skin’s ability to repair. As a result, you might also notice that the skin in your lower leg appears scaly, hardened, or bumpy. The characteristic skin changes associated with venous insufficiency are called stasis dermatitis.
-
Open Wounds (Venous Stasis Ulcers)
Fluid accumulation, lack of circulation, and compromised skin health can cause open sores on your legs that heal slowly. While the wounds themselves may not be particularly painful, venous stasis ulcers can take months or years to resolve, even with medical intervention. Varicose vein treatment significantly reduces your risk of venous stasis ulcers.
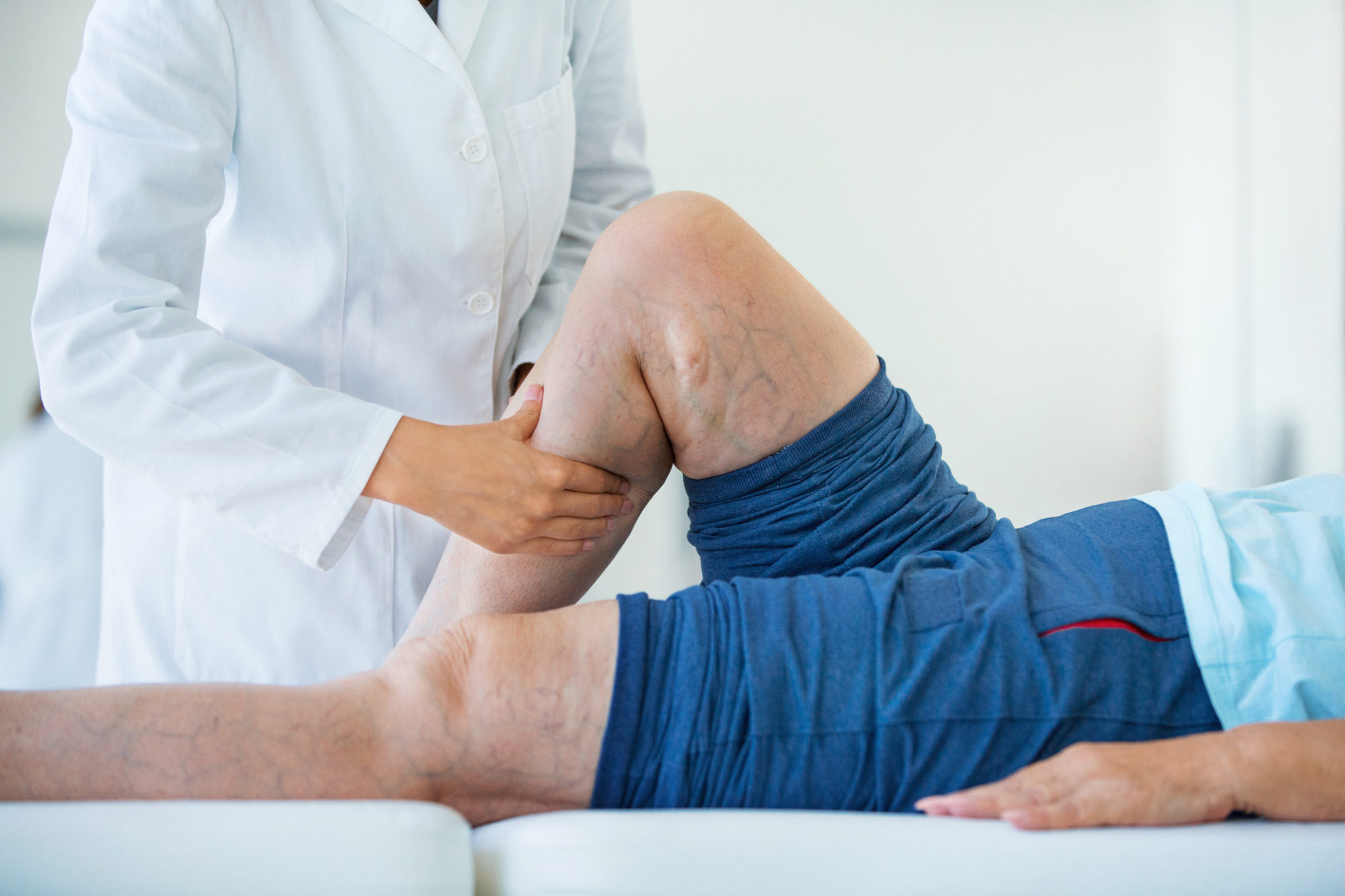
Over-the-Counter Treatments are Unlikely to Provide Significant Results
If you are currently living with varicose veins, you may be tempted to try one of the numerous over-the-counter products promising to alleviate the discomfort or improve the appearance of your legs. While a significant number of product manufacturers are making astounding claims, it’s important to know that the topical application of creams or lotions are unlikely to provide any noticeable results, even if they contain a potentially promising list of ingredients.
The manufacturers of topical creams and ointments containing ingredients like vitamin k, horse chestnut, or butcher’s broom claim their products penetrate the skin to reduce inflammation and strengthen vein walls. Many claim their products reduce the appearance of problematic veins over time. It’s important to know that topical products are not likely to penetrate your skin and cannot reduce the size of varicose veins. Over-the-counter topical products simply cannot address the cause of venous insufficiency, faulty valves and increased internal pressure from the backflow of blood and fluids.
Treating Varicose Veins with Graduated Compression
If you have varicose veins, your doctor will likely recommend wearing graduated compression stockings. Compression stocking help control the detrimental effects of gravity by supporting your legs and assisting vein function. The continuous pressure also helps keep blood and fluids from accumulating in damaged veins. The compression is strongest at the ankle and gradually decreases toward the top of the stocking.
Compression stockings are worn the entire time you are awake, unless otherwise directed, and are commonly prescribed for spider veins, varicose veins, and deep vein thrombosis. While compression stockings will not cure varicose veins, they can slow the progression of the disorder and minimize discomfort. Compression stockings are most effective when donned immediately upon waking before fluids have the opportunity to accumulate in your lower legs.
Minimally-Invasive Intervention for Varicose Veins
As potentially debilitating as varicose veins can be, far too many people are hesitant to seek treatment. Some mistakenly believe that their condition will improve with time, while others assume varicose vein treatment requires hospitalization. While most vein treatments today are done in-office, the concerns about hospitalization are understandable.
Not that long ago, the only effective method of treating diseased veins did require hospitalization. Surgeons tied off diseased veins and removed them. This method of vein treatment, vein stripping and ligation, required the use of general anesthesia and recovery could take several weeks. While vein stripping is still used in certain situations, there are several minimally invasive procedures that eliminate the need for general anesthesia and hospitalization. Most people can return to their usual activities within 24-48 hours after treatment.
Minimally invasive vein treatment can alleviate the pain and discomfort of varicose veins, help ulcerations heal, and allow you feel much more comfortable with the appearance of your legs. If you have varicose veins, your doctor may recommend one of the following treatment options based on the size and location of your varicose veins:
-
Radio Frequency (Venefit™ VNUS Closure™)
This non-surgical treatment option uses a radio frequency (rf) powered catheter to heat the collagen in varicose veins. The procedure is known as radiofrequency ablation. During radiofrequency ablation, heat causes the collagen in the vein wall to collapse, sealing the vein. The procedure is performed under a local anesthetic, and you will likely be allowed to return to your normal activities within a day or two. The procedure itself typically takes about thirty minutes and has an excellent history of long-term success.
-
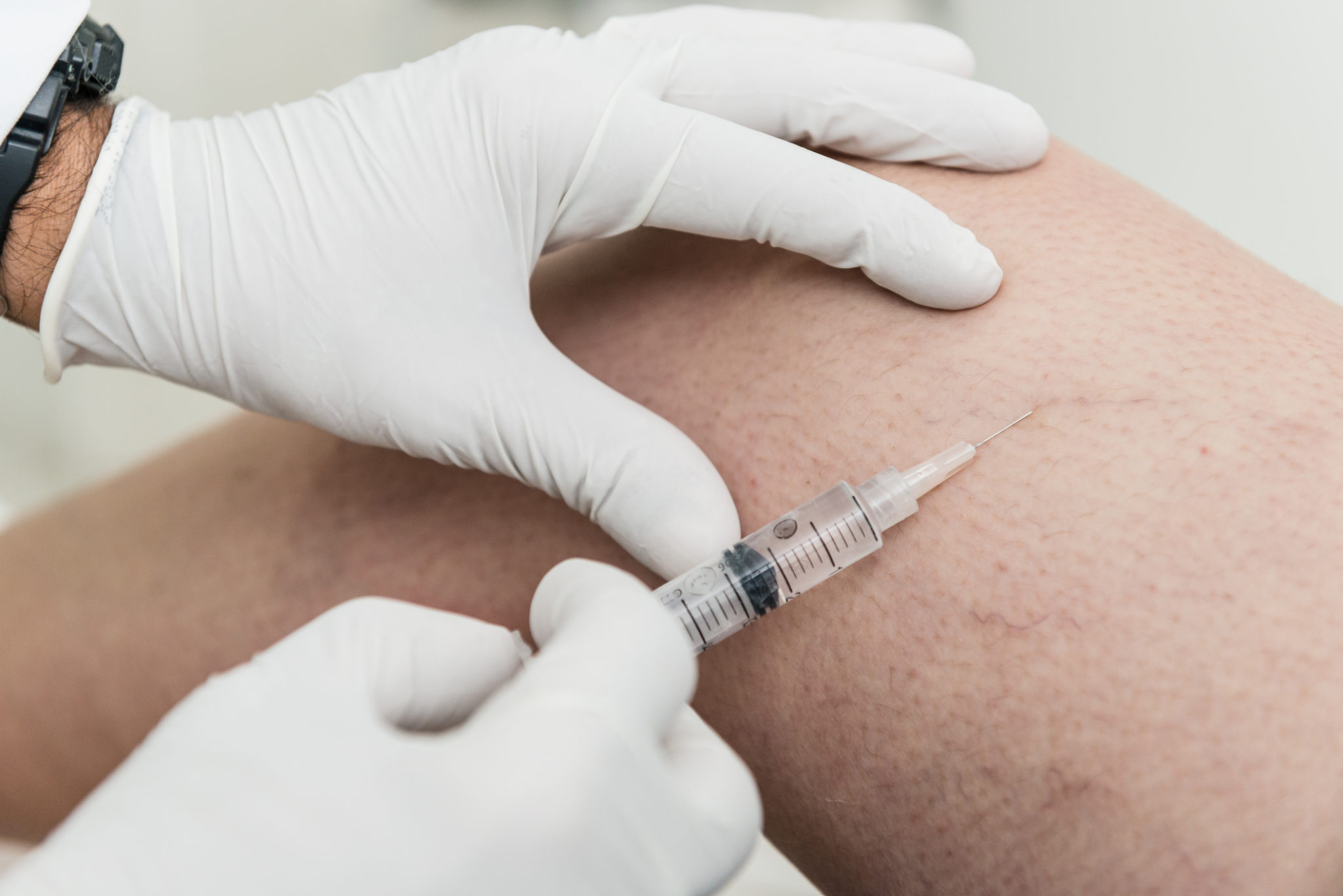
Sclerotherapy
During Sclerotherapy treatment, your physician will inject an irritant into your vein. The irritant causes the vein to shrink and only takes a few minutes to perform. While saline was once the most commonly used solution for sclerotherapy, many treatment centers today are using Asclera®, a safer, more comfortable alternative to saline that causes the capillary walls to collapse and adhere, turn to scar tissue, then disappear. Asclera® can be used for spider veins and varicose veins measuring 3mm in diameter or less.
-
Ambulatory Phlebectomy
This relatively common treatment method allows your vein-care specialist to remove varicose veins through small pinhole punctures in your skin. The incisions will not require stitches. The procedure is done in your provider’s office using a local anesthetic. Most often, those recovering from a phlebectomy are back to their usual activities within 24 – 48 hours of their procedure.
-
Ultrasound-Guided Microfoam (Varithena®)
Varithena® is the only foam approved by the FDA to treat the great saphenous vein, the long vein that runs from your foot to your thigh. Unlike radiofrequency, the Varithena® (polidocanol injectable foam) System does not require the use of a catheter or heat. Since the foam is highly visible in ultrasound imaging, your doctor can position this injectable foam precisely where it is needed. The foam creates a barrier that displaces blood within the diseased vein, causing the vein to collapse. Varithena® treatment is an in-office procedure that is commonly performed in less than 30 minutes.
-
VenaSeal™ Closure Treatment (Cyanoacrylate Closure)
VenaSeal™ is often referred to as the “superglue” vein alternative. During VenaSeal™ treatment, your physician will use ultrasound imaging to determine the ideal location for vein closure. A small, painless catheter will be inserted into the affected veins after the injection site is numbed. The catheter is used to deliver a medical-grade adhesive in specific areas along the diseased vein. Once the adhesive is in place, pressure is applied to help seal the vein, and the catheter is removed. The adhesive used during VenaSeal™ treatment permanently seals the diseased vein.
What to Expect After Varicose Vein Treatment
After vein treatment, your blood flow is redirected to healthy veins. The treated veins collapse and are absorbed into your body. The absorption process can take several weeks or several months, depending on the method of treatment selected and the size of the diseased vein.
There have been numerous advances in varicose vein treatment. While most of today’s treatment methods are minimally invasive and complications are rare, its still important to follow your doctor’s instructions when caring for the treatment area. Your physician will likely advise you to wear compression stockings for a few days or weeks to help with the healing process. Compression legwear is not required after VenaSeal™. Your doctor may also recommend frequent activity throughout the day to improve circulation and reduce the risk of complications. Most often, you will be asked to refrain from vigorous exercise for a week or so.
Varicose Veins Will Not Resolve on Their Own
While varicose veins affect up to 30 percent of the population, many people don’t realize that varicose veins are a progressive condition that can eventually cause skin ulcerations and make walking difficult. Only a small percentage of those living with varicose veins seek treatment before significant complications arise. Those who delay treatment are often unaware of the many minimally invasive options that would allow them to return to their usual activities within a few days of their procedure.
Those painful, bulging, twisted veins on your legs are not likely to improve on their own. For state-of-the-art vein treatment in Henderson, NV, contact Vegas Valley Vein Institute. At Vegas Valley Vein Institute, you will benefit from our comprehensive approach to traditional and non-surgical varicose vein treatment and the medical expertise of Dr Irwin Simon, the Valley’s leading vein care specialist.