A Beginner’s Guide to Varicose Veins
Varicose veins are a common health condition that affects millions of people around the world. In fact, an estimated 25% of all adults have varicose veins.
If you or a loved one have varicose veins, or if you are interested in preventing the development of varicose veins within your body, you may have many questions about this condition, such as:
- What exactly are varicose veins?
- How do they develop?
- What are the risk factors associated with varicose veins?
- What are the different types?
- What are some common symptoms of varicose veins?
- How are they treated?
- What strategies for prevention are most effective?
This beginner’s guide to varicose veins will answer these and other questions that you may have. First, let’s understand what varicose veins actually are.
What are Varicose Veins?
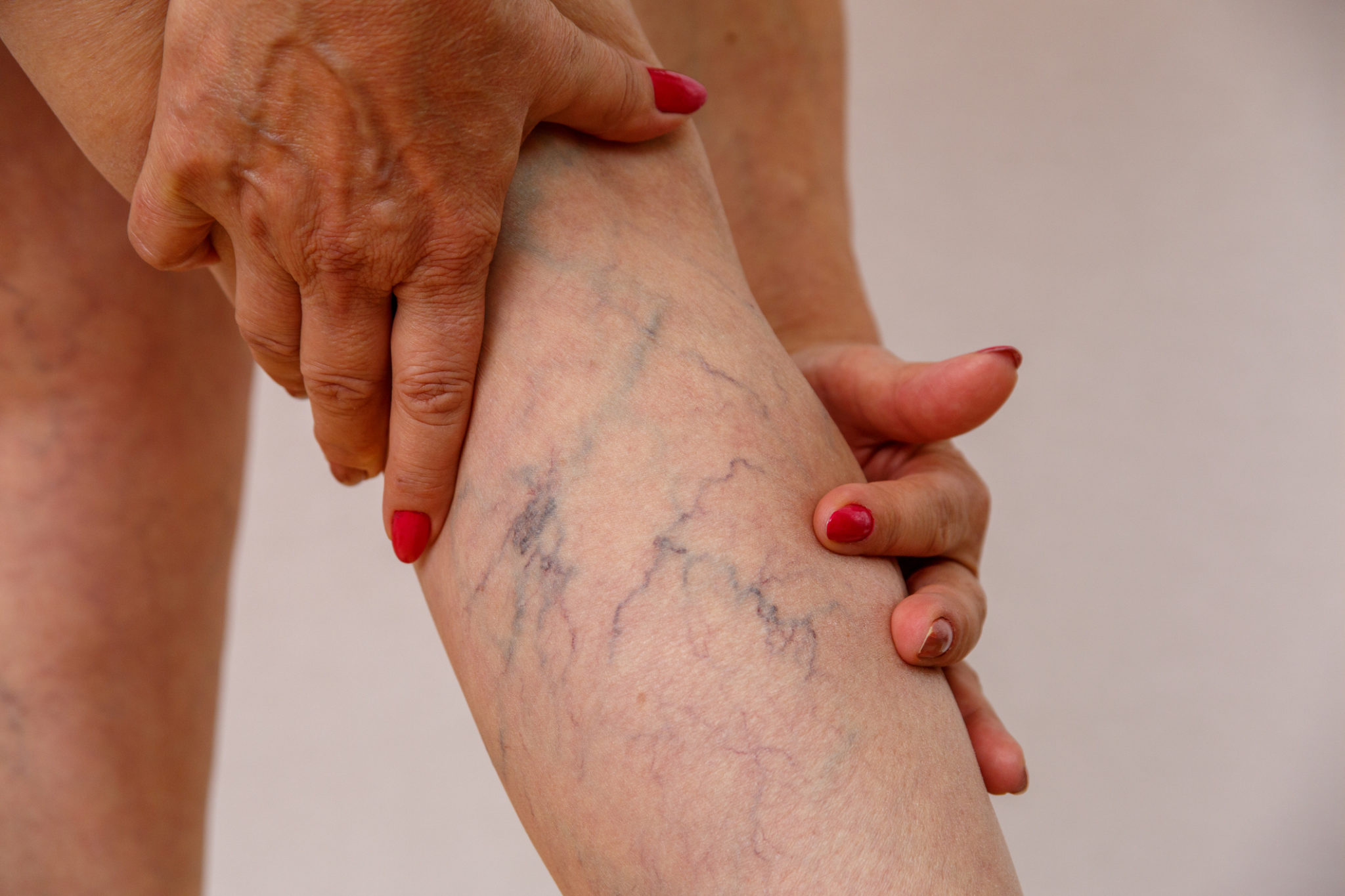
Varicose veins are also referred to as varicoses or varicosities. Varicosities develop when the veins stop working as they should, especially with regards to blood circulation. How are varicose veins different from normal veins?
In normal veins, one-way valves continuously alternate between an open position, which allows blood to circulate “uphill” towards the heart, and a closed position, which prevents backflow. However, in varicose veins these valves do not function properly, and the end result is a pooling of blood within the vein. In turn, this pooling contributes to the congestion of blood flow, and causes the vein to swell and twist.
In most cases, varicose veins can be found in the legs, although they are by no means limited to that region of the body. Since superficial veins have less muscle support than deep, interior veins, they are more likely to suffer from varicosity. When these superficial veins become varicose, they usually manifest as raised, bluish-purple or red-hued channels under the skin that are clearly visible to observers. For the most part, superficial varicose veins are harmless.
On the other hand, when deep-seated veins become varicose they are usually not visible to the naked eye, but can cause swelling and aching throughout the leg or affected region, and even result in the formation of dangerous blood clots. While this is a relatively rare occurrence, it is important to be alert to the possibility of an interior vein becoming varicose.
How do Varicose Veins Develop?
There are several potential causes of varicose veins. In many cases, excessive pressure on the legs or abdominal region is a major contributor to the formation of varicosities. When the skeletal muscles around the veins that help pump blood back to the heart are frequently overworked, it is more likely that varicosities will develop.
In contrast, muscles that are weak or out of prime condition can also contribute to the formation of varicose veins. Thus, occupations that require workers to stand for long periods of time and mostly sedentary office jobs can both pose significant risks for the development of these venous abnormalities.
Some common risk factors associated with the formation of varicose veins include:
- Age. Over the years, the wear and tear brought about by the pumping action within your veins can eventually result in the loosening of those important valves that regulate blood flow. Adults over 50 years of age are especially at risk for varicose veins.
- Gender. Women are generally more susceptible to the development of varicose veins than men are.
- Previous injuries. Leg injuries that damage the valves within the venous system often result in varicosities.
- Pregnancy. Pregnant women have a higher volume of blood in their body than those that are not carrying a child, which means that extra stress is placed on the circulatory system. In addition, as the uterus grows increased pressure on the mother’s pelvic area can result in the formation of varicose veins, which may or may not disappear after the pregnancy is over.
- Menopause. Women undergoing menopause experience changes in their hormone levels. Upon their release into the bloodstream, many female hormones cause vein walls to relax, which in turn contributes to the weakening of the valves that regulate blood flow.
- Certain medications. Hormone treatments like birth control pills can also lead to the relaxation of vein walls and the subsequent formation of varicosities.
- Heredity. Adults with a family history of varicose veins are more likely to deal with varicosities themselves.
- Obesity. Overweight and obese persons have additional pressure on their venous system.
- Long periods of standing. Workers that have to stand for hours at a time often suffer from varicose veins, since blood circulation is generally poor when the body stays in the same position for a long time.
- Long periods of sitting. Office workers also are at risk for varicose veins, because they are frequently required to sit at a desk in the same position for hours at a time. In addition, a sedentary job is often associated with lack of exercise, and even a few hours of sedentary time can cause a significant decrease in overall cardiorespiratory fitness.
The Different Types of Varicose Veins
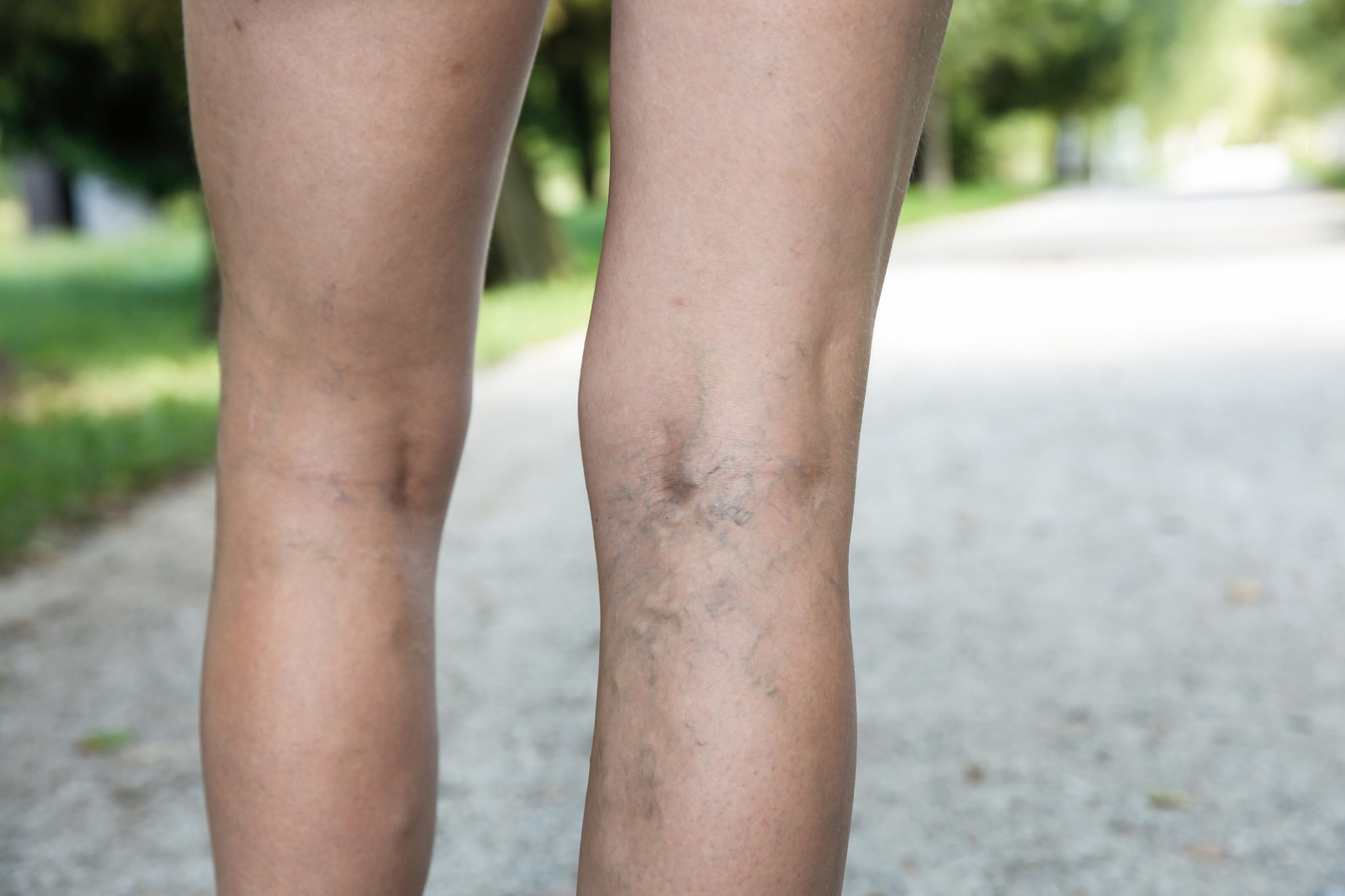
There are several kinds of varicose veins that can manifest themselves throughout the body. The different types of varicose veins include the following:
Superficial Veins
Superficial veins are veins that reside close to the surface of the skin. Superficial vein varicosities are typically harmless, although they can cause itchiness, aching and swelling when inflamed. When varicosities occur in the network of superficial veins, they generally manifest in one of three venous categories:
- Saphenous varicose veins. These varicose veins in the leg have the appearance of very large, rope-like ridges as they bulge out from the skin. However, they are often colorless.
- Reticular varicose veins. Instead of forming large ridges, reticular varicose veins spread out under the skin like a mesh. They are generally red-, green- or purple-hued.
- Spider veins. Spider veins are actually dilated capillaries on the skin. They are thinner and smaller than other types of varicose veins, and are commonly found throughout the body, instead of just the legs. Instead of the appearance of a mesh, spider veins generally form a web-like network of varicosities.
Interior Veins
On rare occasions, interior veins can suffer from varicosities. These can cause significant discomfort and aching throughout the affected area (generally in the leg). If you suspect that you are suffering from an interior varicose vein, it is recommended that you visit your doctor to explore treatment options.
Hemorrhoids
Hemorrhoids (also known as piles) are actually varicose veins located in the rectum and anus. When these veins swell because of fluid retention, the result is discomfort and/or pain during bowel movements. Interestingly, those that suffer from frequent hemorrhoid flare-ups are more likely to develop varicose veins in other parts of their body, since the root cause (weak/improperly functioning valves) is the same in both situations.
Varicoceles
Varicoceles are varicose veins located within the scrotum. According to one estimate, varicoceles can be found in approximately 15% of the adult male population. While varicoceles may not require any treatment, in some cases they may result in a chronic, aching pain within the scrotum, and even infertility.
Symptoms of Varicose Veins
There are several symptoms of varicose veins, ranging from purely cosmetic manifestations to intensely painful conditions. Symptoms could include:
- Discolored or misshapen veins. This is a merely cosmetic condition that results from a venous irregularity. Superficial varicose veins, while generally harmless, are very noticeable to the naked eye.
- Sore or tender legs. Those who suffer from varicose veins may find themselves dealing with frequent soreness in their legs, especially after sitting or standing for a long period of time.
- Swollen ankles. Ankle inflammation is another common indicator of venous abnormalities in the legs.
- Legs that feel heavy. This symptom is especially common after an exercise session, or at night time.
- Lipodermatosclerosis. This refers to the condition in which fat under the skin just above the ankle hardens, resulting in skin shrinkage.
- Venous eczema. Skin around the area of the varicosity is dry, irritated, and itchy.
- Restless legs syndrome. Many adults who have varicose veins also suffer from restless legs syndrome.
- Bleeding. In some extreme cases, the skin around varicose veins may tend to bleed easily.
- Venous ulcers. Venous ulcers often form around the ankles, and are preceded by discoloration in the general area. In some cases, the ulcer that forms does not cause any pain. However, in other situations (such as a case of infection) the ulcer can be extremely painful.
Varicose Vein Diagnosis
In many cases, doctors are able to diagnose varicose veins from a visual examination of the affected area. For instance, raised and discolored veins in the leg would be obvious indicators of a venous abnormality.
Nevertheless, for a thorough clinical examination there are a number of diagnostic tests that can be performed to pinpoint the root cause of the symptoms. These tests could include the following procedures:
- Your doctor may perform an ultrasound to determine how well your blood is circulating. This is a totally non-invasive technique.
- Your doctor may also perform a venogram. In this procedure, special dye is injected into your legs, and X-rays of the affected area are taken. An examination of the dye flow as captured by the X-rays can help your doctor to check the effectiveness of your body’s blood flow.
- The Brodie-Trendelenberg test is a diagnostic procedure that can help your doctor to distinguish between a superficial varicosity and a deep venous insufficiency. In this test, the patient’s leg is elevated, time is allowed for the venous system to “drain,” and then a tourniquet is applied to the mid-thigh. The speed and level of venous refill upon the patient standing upright will indicate to the doctor whether there are superficial venous irregularities at work, or deeper venous insufficiencies that must be addressed.
- The Perthes test, like the Brodie-Trendelenberg procedure, makes use of a tourniquet – this time to help distinguish between a deep venous insufficiency and an obstruction.
Prevention of Varicose Veins
While there is no way to totally guarantee the prevention of varicose veins, there are certain activities that promote good circulation and can reduce the odds of developing venous abnormalities.
For instance, developing a good exercise routine is an excellent way to boost blood flow within your circulatory system. Along with regular exercise, a good diet is essential; especially a low-sodium, high-fiber diet.
It is also good to avoid standing or sitting in the same position for long periods of time. Try to move around or shift position at regular intervals.
Self Treatment Options for Varicose Veins

If you are already dealing with varicose veins, what treatment options are available to you? While most cases of varicose veins do not require treatment, you may want to consider implementing the follow actions:
- Wear compression stockings. Compression stockings are designed to help your legs push blood upwards. They offer the strongest support at the ankles, and gradually loosen as they ascend in the direction of your abdomen and heart.
- Elevate your legs for 10-15 minutes at regular intervals throughout the day. This will help direct your blood flow towards your heart, and also work to counteract blood pooling in your veins.
- Make appropriate lifestyle changes. These could include committing to a regular exercise routine, changing your diet, or losing weight.
Consult Your Doctor for Treatment Options
Apart from self treatment options, you may want to consult with your doctor about additional methods of treating varicose veins. The following list contains a sample of the different options available:
- Radio frequency ablation. This is a minimally invasive alternative to surgical stripping of the Greater or Lesser Saphenous Vein, and utilizes radiofrequency to heat and seal diseased veins. It is known to be a highly effective treatment for venous reflux disease.
- Varithena(R) (microfoam chemical ablation). Varithena is an FDA-approved method of treating the Greater Saphenous Vein (GSV) for varicose vein disease. It does not require a catheter to close the vein, or any form of heat delivery, and is highly effective in treating complicated problems related to varicose veins.
- VenefitTM. Venefit is a non-surgical alternative for treating varicose veins. The procedure involves the application of radiofrequency (RF) energy to heat and contract collagen located inside vein walls. As a result, the vein collapses and is sealed shut. Subsequently, blood flow is naturally redirected to healthy veins.
- Injection sclerotherapy. This procedure involves the injection of an irritant directly into the varicose vein, causing it to shrink in size. Patients that undergo this procedure will often notice immediate relief of physical symptoms.
At the Vegas Valley Vein Institute, we offer a wide range of non-invasive treatment options to our patients, as well as all of the most advanced surgical techniques for eliminating varicose veins. We can help you to implement a comprehensive treatment plan that will either reduce or completely eliminate varicosities from your body, and your life.
If you’d like to learn more, reach out to us at the Vegas Valley Vein Institute today. Let us assist you in making the best possible treatment decision for your varicose veins.