Recognizing and Healing Venous Stasis Ulcers
Your circulatory system relies on nearly 100,000 miles of blood vessels to deliver oxygen and nutrients throughout your body. While the blood-flow through your arteries is powered by the pumping of your heart, the veins directing blood back to your heart and lungs rely on a series of one-way valves. These valves defy the pull of gravity to keep your circulatory system functioning efficiently.
In healthy veins, these valves close completely to keep your blood from flowing downward towards your feet. When valves malfunction due to defect or disease, they can eventually cause a significant amount of discomfort and distress. Left untreated, vein disease can lead to a number of chronic health complications, including venous stasis ulcers.
Understanding Venous Stasis Ulcers
Venous stasis ulcers are wounds caused by the accumulation of fluid that commonly accompanies vein disorders. As fluid leaking from dysfunctional veins accumulates into surrounding tissues, the flesh surrounding the area becomes irritated, inflamed, and begins to break down. Over time, the breakdown of tissues combined with the lack of oxygen and nutrients causes ulcers on the lower leg. The lack of circulation impairs healing. Left untreated, venous stasis ulcers can cause a significant number of health complications, including severe infections and necrosis.
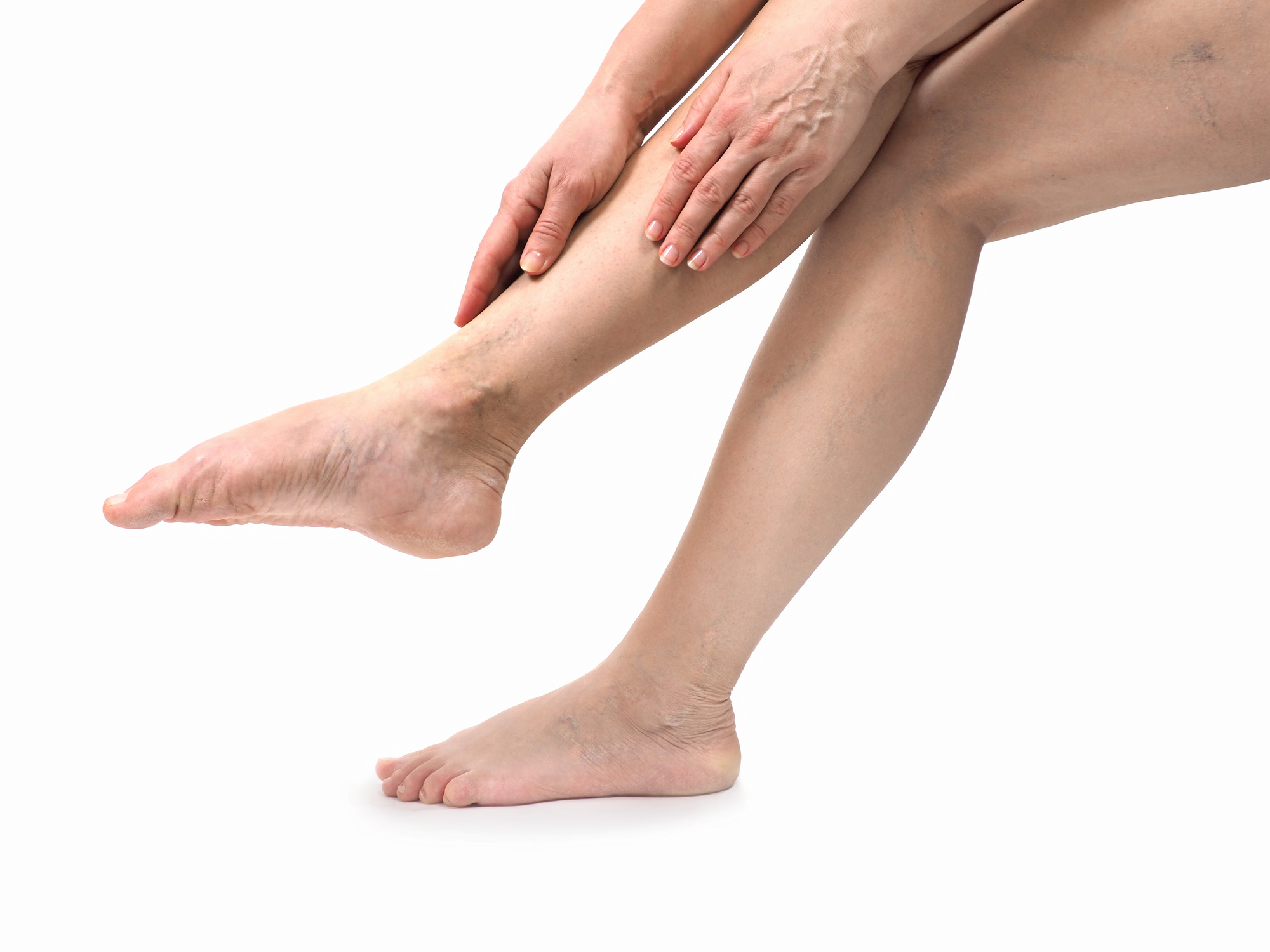
How Venous Stasis Ulcers Evolve
Healthy vein function depends on the contraction and expansion of muscles throughout your body to keep blood circulating from your feet to your heart. As muscles contract blood moves forward. As muscles relax, the one-way valves within your veins form a tight seal to keep blood from slipping backward until the next surge of forward momentum.
When the valves inside your veins lose their ability to form a tight seal, a condition known as chronic venous insufficiency, blood and accumulated fluids seep downward as muscles relax. As veins take on more fluids than they can withstand, the increase in pressure causes the veins in the affected area to stretch and bulge. The first visible signs of venous insufficiency are often spider veins or varicose veins.
Under the additional pressure from blood pooling in the lower leg, the smaller blood vessels begin to leak plasma, proteins, and blood cells. The surrounding tissues swell from fluid accumulation (edema). As protein deposits starve the affected areas of nutrients and oxygen, fluid accumulation interferes with the removal of waste products.
Before the onset of venous stasis ulcers, those affected by venous insufficiency may notice swelling, changes in skin pigmentation, changes in skin texture, or any combination of these symptoms.
Recognizing the Signs, Symptoms, and Stages of the Disease
As a complication of venous insufficiency, venous stasis ulcers affect an estimated 25 percent of our population. The signs and symptoms of venous insufficiency are commonly classified into three distinct phases. The phases of the disorder progress over time, particularly if this chronic health condition is left untreated or poorly managed. The three stages of venous insufficiency are identified by the following symptoms:
-
Venous Insufficiency Stage 1
One of the earliest symptoms of chronic venous insufficiency is varicose veins, the appearance of dark, rope-like veins most commonly appearing in the lower leg. While many people initially consider the appearance of varicose veins little more than an uncomfortable cosmetic issue, as the condition progresses, varicose veins can cause a significant amount of discomfort. In addition to the appearance of twisted, bulging veins, fluid accumulation can cause a general feeling of heaviness in the legs, itching, tingling, and swelling of the feet, ankles or calves.
-
Venous Insufficiency Stage 2
As the symptoms of venous insufficiency progress, the discomfort can be more pronounced. As a result of the breakdown of iron in the blood, skin can turn various shades of red and brown. The skin on the lower leg eventually starts to show outward signs of the internal dysfunction. Skin may appear thickened, hardened, scaly, or bumpy, a skin condition known as stasis dermatitis. As inadequate blood supply impairs the skins ability to regenerate, even mild trauma or scratching can injure traumatized skin. Those living with chronic venous insufficiency may also find their skin can appear thin, shiny, weepy, or crusty. Since venous insufficiency impairs the healing process, skin damage can easily become infected.
-
Venous Insufficiency Stage 3
Venous Stasis ulcers commonly occur during the third phase of venous insufficiency, open sores that fail to heal. Venous stasis ulcers commonly begin as a small sore on the surface of the skin but can quickly expand. The most common location for venous ulcers to appear is near the ankle, but they could appear anywhere on the lower leg. Venous ulcers that form above the ankle are often the result of skin trauma or scratching. While ulcerations can cause a significant amount of pain, many find the wound itself relatively painless unless infection sets in. With proper treatment, venous ulcers can heal, but healing can take a considerable amount of time.
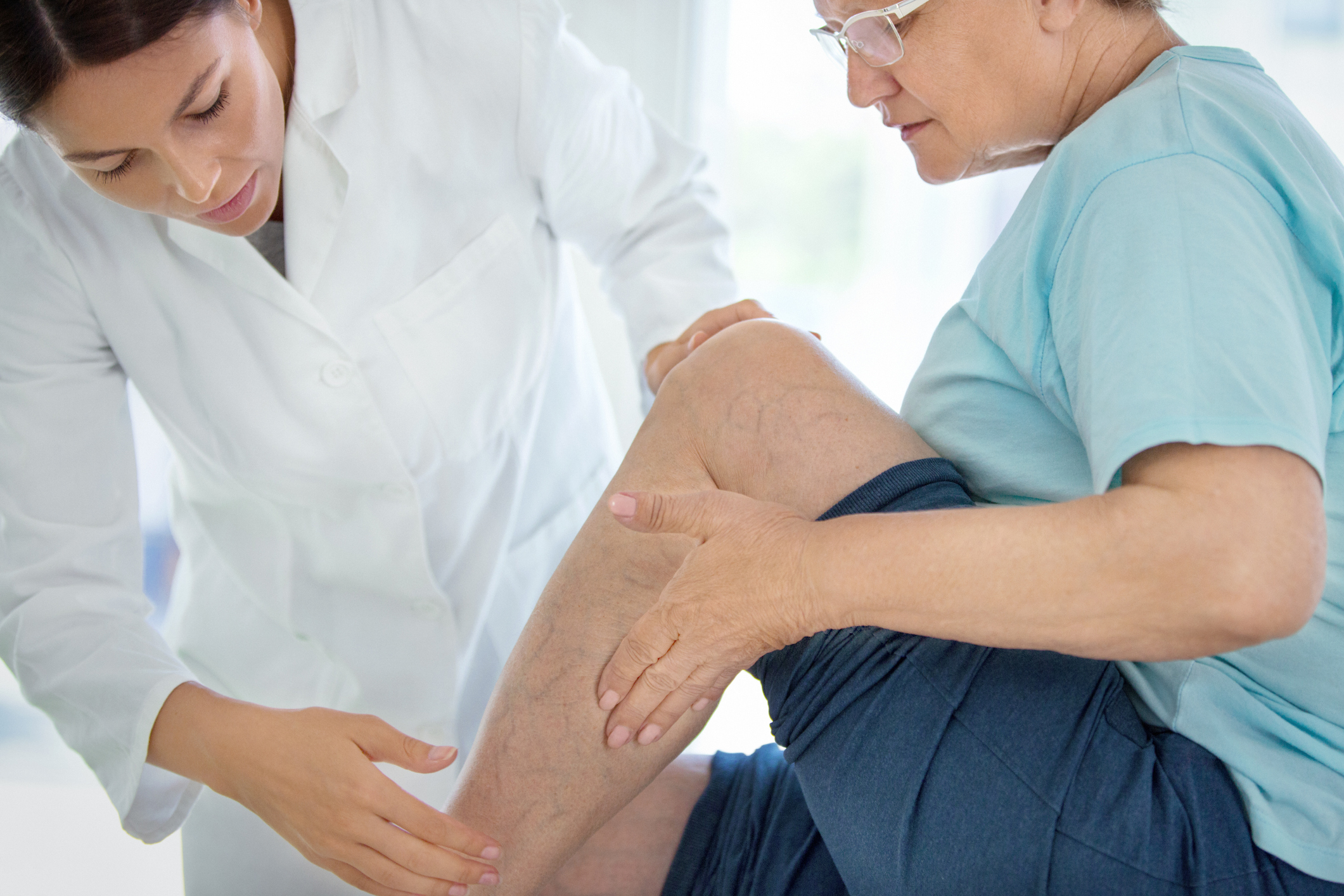
Those Most at Risk of Developing Venous Stasis Ulcers
While having varicose veins increases your risk of developing venous ulcers, chronic venous stasis ulcers can also be the result of a blood clot obstructing blood flow in the deep veins of the leg, deep vein thrombosis (DVT). When venous ulcers develop because of a blood clot, the resulting condition is known as post-thrombotic syndrome. While vein disease does not discriminate by age or gender, the condition is more prevalent in those over the age of 50 and more common in women than men.
Knowing the risk factors for developing venous stasis ulcers (VSU) may help you avoid this potentially devastating complication of circulatory issues. There are a significant number of circumstances that increase your risk, including:
- Family history of VSU
- Varicose veins
- History of edema (leg swelling)
- Uncontrolled or undiagnosed high blood pressure
- Previous history of blood clots
- A history of diabetes or diabetic neuropathy
- Congestive heart failure
- Trauma to the legs
Treatment Options for Venous Stasis Ulcers
At first, venous ulcers are generally shallow and irregularly shaped. As the deterioration of the affected tissue progresses, the ulcer can extend deeper into the underlying tissues, involving the tendons, ligaments, and bone. The goal of venous ulcer treatment is to minimize edema, control infection, heal the wound, and prevent reoccurrence. Many leg ulcer patients experience alternating periods of healed and open ulcerations. Those with venous stasis ulcer commonly find the skin lesions will return unless the underlying cause is corrected.
To effectively treat venous stasis ulcers, doctors commonly evaluate the venous and arterial circulation in the affected area to identify the underlying cause. Once the cause is determined, physicians are in a better position to develop a successful plan of action. Doctors treating venous ulcers may recommend one or more of the following options:
-
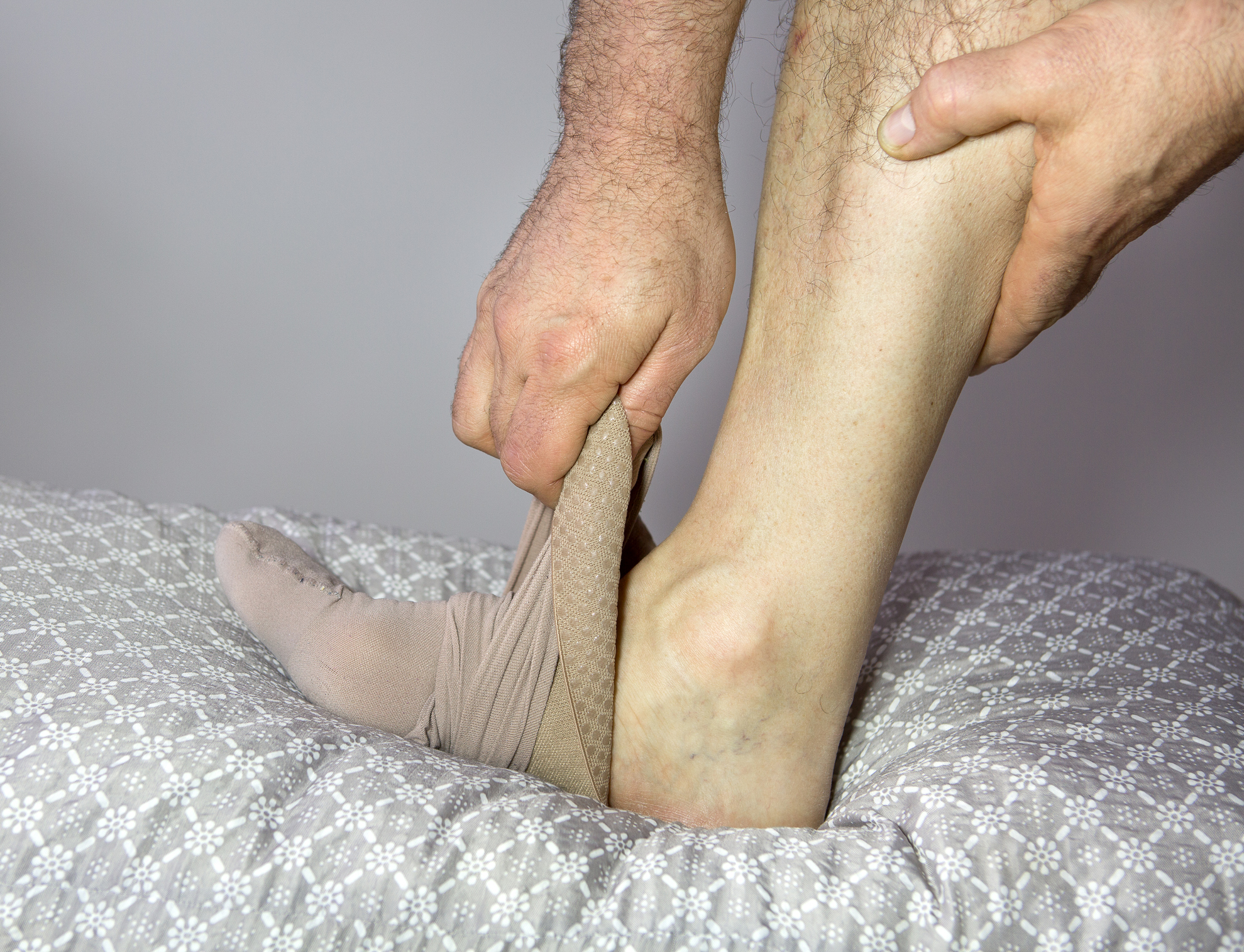
Compression Stockings
Compression stockings are one of the first lines of defense for the treatment of venous ulcers. Graduated compression stockings help minimize swelling and support vein function. Compression stockings also promote wound healing and help reduce the risk of reoccurrence by boosting circulation. Your physician might also suggest covering the wound with a transparent dressing, a clear, plastic-like film worn under the compression stocking to protect the wound and promote healing.
-
Unna Boot Therapy
Similar in function to compression stockings, an Unna boot is created from a moist gauze bandage that securely wraps the affected limb from the toes to just below the knee. The treated gauze commonly contains zinc or a combination of zinc and calamine to fight infection and help the ulcer heal. As the treated gauze dries, it hardens to form a custom-fit, secure boot that helps improve circulation and minimize edema.
-
Topical Preparations
For the discomfort of venous dermatitis, your doctor may recommend using a prescription anti-fungal preparation to prevent the spread of infection. If skin rashes result in an uncomfortable itch, or if scratching causes skin injury, hydrocortisone cream is often prescribed to minimize the risk of further damage. Since topical antibiotics can increase inflammation, they are commonly avoided.
-
Debridement
For an ulcer failing to heal because of infection or tissue damage, wound debridement may be the first step to promote healing. Debridement removes damaged, necrotic tissue from the wound while activating platelets and growth factors in the treatment area. There are several methods of debriding a wound, including chemicals, irrigation, or surgical intervention. In many cases, debridement can decrease the severity of scarring.
-
Vein Ablation
Vein ablation closes off the damaged areas of a diseased vein, redirecting blood flow to a healthy vein. If your vein specialist recommends ablation, they will likely suggest one or more of several available options depending on the location and size of the dysfunctional area. Troublesome veins can be sealed using radiofrequency waves, laser heat, chemical foam, or a glue-like substance.
-
Ambulatory Phlebectomy
Ambulatory phlebectomy is a relatively common method of treating varicose veins close to the surface of the skin. This minimally invasive procedure involves removing damaged blood vessels through small incisions. After a phlebectomy, patients are commonly advised to wear compression stockings to improve circulation. Most people get back to their usual activities within the first 24 hours after the procedure.
Enhancing Your Ulcer Treatment with Conscientious Self-Care
Those at risk of developing venous stasis ulcers should make a habit of checking the condition of their feet, ankles, and legs daily, mindful of any changes in the color or texture of their skin. Once a doctor establishes a treatment plan, it’s important to follow through with any recommended lifestyle modifications. Just a few of the self-care strategies commonly recommended for managing venous ulcers include:
-
Wearing Compression Stockings as Recommended
Whether your physician prescribes knee-high or thigh-high compression stockings, it’s important that stockings are worn consistently. In general, compression stockings are worn from the time a person wakes until they are ready to turn in for the night. When stockings are donned immediately upon waking, there is less opportunity for accumulated fluids to pool in your lower legs.
-
Staying Active
Physical activity promotes vein health. Those who remain active and walk frequently benefit from the pumping action of calf muscles reducing pressure in the veins, oxygenating tissues, and removing accumulated waste products. When walking is not an option, circulation can be enhanced by frequently moving your feet to engage your calf muscles and rotating your ankles. Even short bursts of moderate activity throughout the day promotes healing.
-
Elevating Your Legs
Your vein specialist will likely advise you to elevate your legs above heart-level 3 or 4 times throughout the day. By simply elevating your legs for 15 minutes at a time, you reduce the pressure in your veins significantly. Make an effort to graduate the elevation from your knees to your feet. Placing a single pillow under your feet without supporting your legs could cause your knees to hyper-extend, which can make elevating your legs uncomfortable.
-
Making Healthy Lifestyle Choices
Maintaining a healthy lifestyle has a direct impact on vein health. A nutritious diet, regular exercise, maintaining a healthy weight, and following the recommendations of your health care provider can slow the progression of vein disease, ensure the successful outcome of vein treatment, and promote healing.
Treating Venous Insufficiency Reduces Your Risk of Venous Stasis Ulcers
Venous Stasis Ulcers are often caused by faulty veins in the lower leg. Most often, the condition evolves over time. The first signs of venous insufficiency could include a feeling of heaviness in your legs and the gradual appearance of bulging veins. As the condition progresses, you may notice leg pain, changes in skin color and texture, and ulcerations.
Even with lifestyle modifications, damaged veins are not likely to improve on their own. Left untreated, venous insufficiency can have a significant impact on your overall health and wellbeing. That’s why it’s important to have problematic veins treated before the disease has an opportunity to progress. Even with the best medical care, venous stasis ulcers can take many months to heal and can reoccur. Preventing ulcers is considerably more comfortable than waiting for ulcers and skin damage to respond to treatment.
Significant advances in technology and methodology have made treating venous insufficiency and venous stasis ulcers easier and more effective than ever before. For state-of-the-art vein care in Henderson, NV, contact Vegas Valley Vein Institute. At Vegas Valley Vein Institute, you benefit from our comprehensive treatment approach, traditional and state-of-the-art non-surgical treatment options, and the expertise of the Valley’s leading vein care specialist.
Additional Sources:
https://www.winchesterhospital.org/health-library/article?id=2013166525
https://www.webmd.com/skin-problems-and-treatments/eczema/venous-stasis-dermatitis#2