Varicose Veins Symptoms
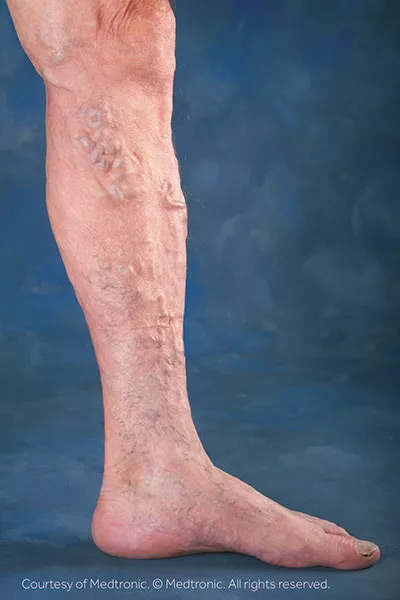
Varicose veins are most often swollen, gnarled veins that most frequently occur in the legs, ankles and feet. Varicose veins are veins with incompetent valves which are elongated, dilated, tortuous, pouched and thickened. They are produced by a condition known as venous insufficiency or venous reflux, in which blood circulating through the lower limbs does not properly return to the heart but instead pools up in the distended veins.
More than 25 million Americans suffer from venous reflux disease. The symptoms can include pain and fatigue in the legs, swollen ankles and calves, burning or itching skin, skin discoloration and leg ulcers. In less severe cases, thin, discolored vessels – “spider veins” – may be the only symptom.
Gender and age are two primary risk factors in the development of venous reflux. An estimated 72% of American women and 42% of men will experience varicose veins symptoms by the time they reach their sixties. Women who have been pregnant more than once and people who are obese, have a family history of varicose veins or spend a great deal of time standing have an elevated risk for the condition, but it can occur in almost anyone at almost any age. Varicose veins never go away without treatment and frequently progress and worsen over time.
What Causes Varicose Veins?
In veins that function normally, blood flows to the heart and valves within the vein prevent the blood from flowing backward. A varicose vein occurs when the valves do not completely seal and blood begins to seep back the other way. Blood pools in the vein, increasing venous pressure and weakening the vein wall. Over time, this 6causes leg swelling and permutation of the superficial vein.
In some cases, varicose veins are a precursor of a potentially dangerous condition known as Deep Vein Thrombosis (DVT). If you are experiencing any of the symptoms listed below and suspect that you have a varicose vein, it is important to seek evaluation from a vein specialist like Dr. Simon.
ARE YOU EXPERIENCING SWELLING? SCHEDULE YOUR APPOINTMENT NOW!
Am I at Risk for Varicose Veins?
There are many factors that can contribute to the development of varicose veins and other venous diseases.
Age
Heredity
Pregnancy
Hormone Changes
Obesity
Occupations that require standing or sitting for long periods
Exposure to sun on fair skin
Injuries to the skin's surface
Bruising
Can I prevent varicose veins?
While there is no way to completely prevent varicose veins and other venous diseases, you can make some measures to help drive optimum vein health. Be active. Low to moderate impact aerobic activity such as walking, cycling, jogging and swimming are easy ways to get blood flowing and improve circulation. If you are experiencing some mild symptoms already, the use of compression hose can prevent blood from pooling in the leg veins.
© 2016 - 2017 Vegas Valley Vein Institute